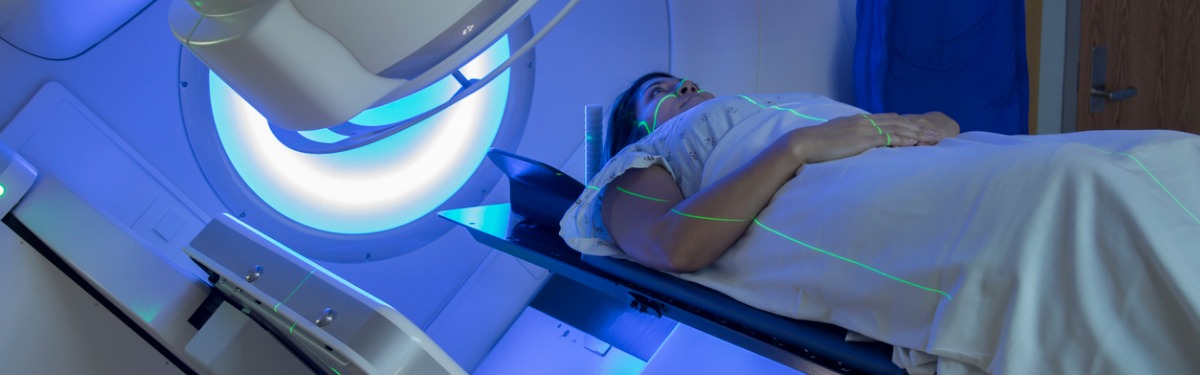
A simple technique in which patients hold their breath for up to 20 seconds to spare the heart from radiotherapy during breast cancer treatment has been adopted as the standard of care across many UK hospitals.
Published: 31 August 2022
Breast cancer radiotherapy is linked to heart disease
Improvements in the detection and treatment of breast cancer mean that many more women are living long enough to experience side effects from their cancer treatment years later. One of these side effects is a small increased risk of heart disease following radiotherapy for cancer in their left breast.
More than 60% of patients receive radiotherapy as treatment for breast cancer, either routinely after removal of lumps or selectively after a mastectomy. Radiotherapy itself has contributed to halving deaths from breast cancer since the 1970s but, in some cases, it can also expose the heart to harmful radiation.
Using older radiotherapy techniques, the risk of death from radiation-related heart disease was as high as 2%, particularly in women with underlying risk factors. Finding ways to reduce the radiation dose to the heart and thereby minimise the risk of heart disease was therefore a priority for the NHS.
In 2012, the NIHR Research for Patient Benefit Programme funded a team of researchers at The Royal Marsden NHS Foundation Trust to investigate different ways of delivering women’s radiotherapy that might achieve this goal. Led by Dr Anna Kirby, Consultant Clinical Oncologist at The Royal Marsden NHS Foundation Trust, the HeartSpare study focused on breathing techniques and women’s position during treatment.
Previously, patients undergoing breast radiotherapy were treated while lying on their backs and breathing in and out naturally. One alternative is for patients to hold their breath during treatment. When the lungs are full of air, the heart is pulled away from the radiotherapy beam targeting the breast. This technique can reduce radiation doses to the heart by up to 70%.
However, conventionally an expensive device is used to assist the breath-hold during radiotherapy. The device works by monitoring the depth of patients’ breath-hold and signalling the radiographer to begin treatment when ready.
Through the HeartSpare study we wanted to test whether simply asking patients to take a breath in and hold it for up to 20 seconds could reduce radiation doses to the heart as effectively and reliably as device-assisted techniques.
Dr Anna Kirby, Consultant Clinical Oncologist at The Royal Marsden NHS Foundation Trust and lead researcher for the HeartSpare study
Heart-sparing radiotherapy reduces heart damage
The first part of the HeartSpare study compared the simple voluntary breath-hold technique against the device-assisted breath-hold. Twenty-three women who had undergone surgery for left-sided breast cancer at The Royal Marsden were taught to hold their breath (voluntary breath-hold) for about 20 seconds while having radiotherapy. They used this method for half of their course of treatment, and for the other half they used a commercial device to guide their breathing.
The two methods of breath-holding were equally effective in reducing radiation doses to the heart, but the voluntary method was quicker and cheaper. The researchers also found that patients and their radiographers preferred the voluntary breath-hold technique to the device. The results from this study are published in the journal Radiotherapy & Oncology.
The team went on to test whether, in women with larger breasts, treating patients lying on their fronts (prone position) was an effective alternative to the voluntary breath-hold technique. Thirty-four women took part in this investigation, receiving half their treatment in the prone position and the other half of their treatment lying on their backs and using the voluntary breath-hold technique.
Publishing their results in Radiotherapy & Oncology, the team confirmed that breath-holding while lying on their back was the significantly better method for reducing radiation dose to the heart and was also preferred by patients.
The team went on to carry out a trial involving 93 women from 10 hospitals around the UK who had already been recruited to the large NIHR Health Technology Assessment Programme-funded FAST-Forward trial.
This HeartSpare trial found that during their course of treatment, 95% of women received a lower dose of radiation to the heart using the voluntary breath-hold technique than they would have while breathing normally. Each hospital was able to accurately treat patients using the voluntary breath-hold technique. The study’s results, published in Clinical Oncology, confirmed that the voluntary breath-hold was a safe and effective method of minimising radiation to the heart during treatment that could be used in all hospitals.
Improving the standard of care
The team’s demonstration that the low-cost, equipment-free voluntary breath-hold technique could spare the heart from radiation has drawn national and international attention. During the study, over 40 different UK centres and six centres from Australia and New Zealand contacted the team to either participate in HeartSpare or visit the centre to learn the technique. Dr Kirby observed that: “It was extremely encouraging that there was a collective desire in the oncology community to implement heart-sparing breast radiotherapy into routine clinical practice.”
The HeartSpare results informed the 2018 update of the NICE guidelines on breast cancer diagnosis and treatment, in which use of the voluntary breath-hold technique was recommended for adoption across the UK for women of all breast sizes. Use of the technique was considered likely to be cost effective because the costs of implementing it were minimal. Furthermore, fewer patients would go on to develop and require treatment for heart disease.
The technique was adopted by many of the centres participating in the HeartSpare Trial. The research team also delivered national workshops and published a video-based demonstration of the technique, which is accessible from the Journal of Visualised Experiments. The video has been downloaded more than 40,000 times, supporting changes in national and international practice.
A Royal College of Radiologists audit demonstrated that the use of heart-sparing breast radiotherapy techniques across the UK increased from around 6% prior to the HeartSpare study to over 50% after the study. Implementing such techniques as the standard of care across the UK has likely benefited several thousand women with left-sided breast cancer per year. In an editorial co-authored by Dr Kirby and published in Clinical Oncology, the authors estimated that by 2040, heart-sparing radiotherapy techniques could reduce breast radiotherapy-related heart attacks from 19,500 to 6,000 and deaths from heart disease from 9,000 to 2,000.
In an era of spiralling healthcare costs, it has been so exciting to be able to demonstrate that the straightforward act of holding a breath can reduce patients’ risks of late cardiac complications from their breast cancer radiotherapy.
Dr Kirby

