In the UK our ability to access rich patient data within our national healthcare system is rapidly expanding. The advent of the ehealth record and ever-growing interconnectivity of information systems is opening up new opportunities and enabling new and innovative approaches to conducting clinical trials. The SIMPLIFIED study is a case in point and is the first renal registry-facilitated trial of its kind.
Published: 04 October 2019
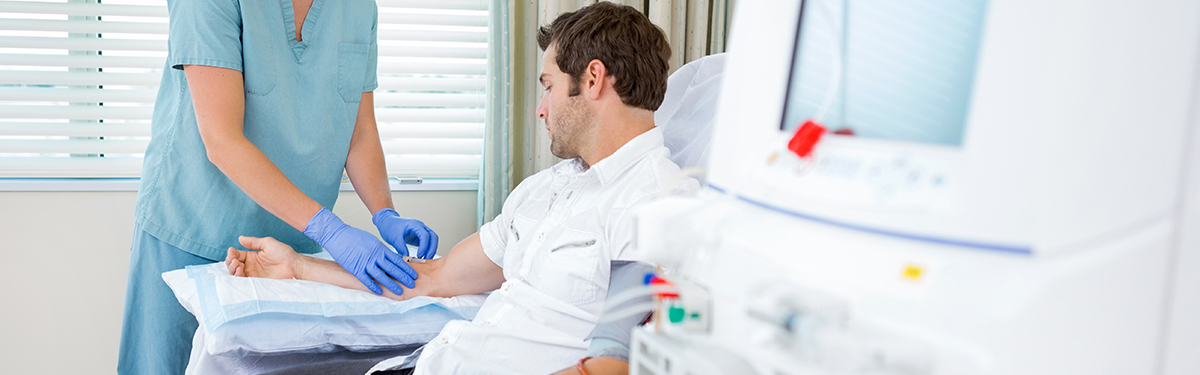
The NIHR research infrastructure supports the delivery of complex and innovative clinical trials.
Rapid access to rich patient data
Clinical need
Vitamin D deficiency is common in kidney failure and is associated with increased risk of death from cardiovascular disease, infections and cancer. Currently only 68% of patients on dialysis will survive for three years or more.
To help address this, dialysis patients receive vitamin D supplements as part of their treatment. Typically, in the NHS, they receive pre-activated vitamin D (an artificial form of vitamin D). However, this increases blood calcium concentrations and may, paradoxically, make vitamin D deficiency worse. International treatment guidelines now recommend that kidney patients receive a natural form of vitamin D (known as cholecalciferol), since we now know that every organ activates vitamin D as required, even in kidney failure.
However, evidence to support this recommendation is severely lacking, and it has not yet been proven through clinical trials. The SIMPLIFIED study will rectify this knowledge gap by testing to see if cholecalciferol can increase the life expectancy of dialysis patients.
Innovative design: The first renal registry-facilitated trial in the UK
SIMPLIFIED opened in March 2017 and aims to enroll 4,200 dialysis patients from across the United Kingdom (UK) and follow them for approximately seven years. Participants are randomly assigned to receive either cholecalciferol or standard care and, as the study is looking at survival, the primary end point is mortality (death). It’s an interventional trial yet it only involves one face-to-face patient visit - which is one of the reasons why SIMPLIFIED is considered the first trial of its kind. Dr Thomas Hiemstra, Clinical Trials Methodologist at Cambridge Clinical Trials Unit and chief investigator of SIMPLIFIED explains why the trial is unique:
It’s unique primarily because all the data capture is done both remotely and indirectly
“SIMPLIFIED is certainly the first nephrology registry-facilitated trial in the UK that we are aware of. It’s unique primarily because all the data capture is done both remotely and indirectly. In other words, all study assessments are conducted using data from information systems that already exist and are already capturing routinely collected clinical information about the participants. So for those patients taking part, this means just one visit to their usual clinic or dialysis centre to enrol in the study and complete the forms which give us consent to access their data. It’s a very efficient way of conducting a clinical trial.”
“It is made possible because SIMPLIFIED is a partnership with the UK Renal Registry, which is a Renal Association initiative. The UK Renal Registry has been collecting, analysing and reporting on data from all dialysis patients from 71 adult and 13 paediatric NHS renal centres since 1995. It was established to help audit, maintain and develop the quality of renal care across the UK. It collects routinely captured clinical data such as: when the patient started treatment and what treatment they receive, as well as their blood pressure and biochemical results (blood test results).
“The Renal Registry is recognised as one of the very few high quality clinical databases that are open to requests from researchers and we can extract data on all of these variables. For SIMPLIFIED participants, this information is collected via an automated process. Data tranches are received daily and the participant’s data is transferred securely into the SIMPLIFIED trial database.”
But SIMPLIFIED also seeks to monitor and analyse other health outcomes that are associated with Vitamin D deficiency. Dr Hiemstra describes how data on these other health outcomes are collected:
“The Renal Registry data allows us to track the renal health of our participants for the duration of the study. But the primary endpoint of the study is mortality and we will determine whether patients are alive or dead at the end of the study from the National Death Register. However, there are other secondary outcomes that we need to capture that are linked to vitamin D deficiency. Plus we also want to be able to compare the quality of life in the two arms of the trial. To collect this information we need to draw data from a number of different data sources.
“For example, any hospitalisations resulting from cardiac episodes, stroke, infections and fractures are determined from Hospital Episode Statistics which are obtained at a minimum of six monthly intervals for the duration of the trial. Whereas new incidences of cancer will be determined from the UK and Ireland Association of Cancer Registries (UKIACR) database at the end of the trial.
All the data is linked together by the participants’ NHS number for sites in England and Wales, and by their CHI number for sites in Scotland
“All the data is linked together by the participants’ NHS number for sites in England and Wales, and by their CHI number for sites in Scotland. This is something that can easily be achieved in the UK because we have one national healthcare system.
“Health-related quality of life is measured using the EQ5D questionnaire, which is completed by participants at six-monthly intervals. When the patient enrols in the study they can choose to complete the questionnaire either by phone call, via a paper copy in the post, or through one of two digital options. The first digital option involves creating their own profile on the study database, which they can do via the internet on a PC or laptop. In addition, we also have a smartphone app. The mean (average) participant age is 70+ so the majority of participants prefer paper or a phone call. However, we are seeing younger participants embracing the smartphone app. The idea is that we make participation as simple as possible – hence the name SIMPLIFIED.”
In addition to the core outcome set described above, some SIMPLIFIED participants grant permission for the study team to collect data from another source. This has created an opportunity to conduct a data experiment within the trial. Dr Hiemstra continues:
“The Renal Association also a key partner of the PatientView initiative, which is provided in collaboration with other partners including the Departments of Health in England, Scotland and Wales. The PatientView initiative is designed to help patients manage long term conditions by giving them real-time access to their health records including blood and urine test results. The laboratories upload test results to PatientView on a daily basis. This is crucial for renal patients to help them manage their phosphate levels, which they do by adjusting their diet.
“When a patient who uses PatientView enrols on SIMPLIFIED, they give permission for us to access this data. Once the patient is randomised their records become part of an automated daily data run and within 24 hours those biochemistry results are imported securely into the trial database.
Once the patient is randomised their records become part of an automated daily data run and within 24 hours those biochemistry results are imported securely into the trial database.
“We have recruited more than1800 participants (as of November 2019) and about 60 percent of them are registered with PatientView. This allows us to monitor the blood calcium levels of those patients, which can have an effect on vitamin D deficiency. It also means we don’t need to conduct separate blood tests specifically for the trial. This was never intended as a core outcome measure of SIMPLIFIED, but it adds another dimension to the data which could provide further valuable insight or evidence in relation to our research question.”
NIHR support
SIMPLIFIED is currently being delivered at 47 sites (England: 43; Scotland: 2; Wales: 2), with more sites about to open. The efficient design of the study means that NIHR support at site level is only required when enrolling patients.
Nottingham University Hospitals NHS Trust (City Campus) is leading the way in recruitment with 176 patients enrolled (as of 24 October 2019) which by far exceeds the site target of 100 patients. Sarah Brand, Senior Research Nurse, works as part of the small team at this site which is part-funded through the NIHR Clinical Research Network to deliver renal research. Sarah believes the recruitment success is largely down to the design of the study:
“It is a ‘simple’ study to recruit to for a number of reasons. From the patient’s perspective it is low risk as they will receive either standard care or an additional vitamin. But equally important is the fact that the burden of participation is low. This is very important because the treatment burden for dialysis patients is very high - three visits a week to the dialysis unit for several hours each time. For SIMPLIFIED there are no additional clinic visits or blood tests and the trial medication is given when they come for dialysis, so participants don’t even need to remember to take any additional pills. Pragmatic trials are good in this way because they are designed to evaluate the effectiveness of an intervention in real-life routine clinical practice conditions.
“The patient information and consent forms are also very straightforward. I usually spend 15-20 minutes explaining the study. I then come back to the patient on a subsequent dialysis session, when they have had time to think about it, to see if they would like to participate. There is just one consent form to sign and the initial EQ5D quality of life assessment is only five questions - it’s all very quick and easy.”
From a research nurse perspective, Sarah also cites several reasons that make SIMPLIFIED a low intensity study to deliver:
“The inclusion and exclusion criteria are broad, so it only takes a few minutes to check if a patient is eligible. Another interesting point is that I can effectively recruit to more than one study at a time. We are currently delivering a second registry-facilitated renal study with a similar design but answering a different research question. I tend to discuss both studies with patients at the same time. It’s entirely up to them if they choose to participate in one, both or neither. But more often than not, they choose to participate in both because the burden of participation is so low.
Really well designed studies, like SIMPLIFIED, are easy for both the participants and the clinical team.
“With other trial designs these two studies might be seen as competing for the same patients, whereas I see these trials as complementary. Really well designed studies, like SIMPLIFIED, are easy for both the participants and the clinical team. They can be delivered with minimal resources while answering very important research questions about renal care.”
“I’ve recruited an additional four patients just this week, so we are now at 180 (as of 1 November 2019) against a target of 100. This is partly because of the study design and also because our research team is fully embedded in the renal clinical team. We know how the dialysis unit works and we plan our recruitment activities to fit around the patient’s needs and the clinical routine. This embedded approach helps to optimise our recruitment success. I’m aiming to double our target and enroll 200 participants before recruitment closes.”
Unparalleled access to rich patient data
Of course, registry-facilitated research is not an entirely unique or new concept and Dr Hiemstra acknowledges that other registry-facilitated renal studies have followed in the footsteps of SIMPLIFIED in recent years. But with an ever-increasing burden on our health services, Dr Hiemstra is quick to highlight the benefits of new approaches to how we do research, which are being made possible by the UK’s rapidly expanding access to rich patient data:
“SIMPLIFIED is not just about answering an important question in the care of dialysis patients, it is also about embracing more efficient ways of doing research. It’s about accessing, analysing and extracting insights and evidence from existing data systems, instead of using up research resources to generate new data. We are fortunate in the UK in that we have had one national healthcare system for over 70 years which is unparalleled in terms of a source of rich patient data. If we can utilise that data to save time and resource when conducting research, while simultaneously making participation easier for patients, then it is a win-win situation. Put simply, to develop new and better treatments faster, we need to find new and better ways of doing research.”
More about registry-facilitated trials
In a clinical and research context a registry is a database of clinical data from patients with a particular disease or condition. When patients consent to become part of a ‘research’ registry they are normally:
- allowing all or some of their electronic health record to be anonymised and added to a database;
- and giving permission for that data to be accessed and analysed by investigators for observational research purposes.
Research registries offer enormous opportunities for clinical research and present a very efficient way of conducting studies. One benefit is that investigators can use a registry to identify potential study participants without having to recruit their own cohort of patients, in effect, the recruitment is already done. Registries can also provide access to historical data which spans many years, which enables retrospective longitudinal studies. Some registries also have a mechanism for ongoing collection of data, and can therefore be used to conduct prospective studies.
For the patient there are also advantages, primarily that the burden of participating in studies is low and does not require additional hospital visits over and above their normal treatment or care routine. It also enables participants to take part in multiple studies simultaneously, to help generate clinical evidence and improve our understanding of disease, with the ultimate aim of developing new treatments.
Further information
- Read more renal research case studies demonstrating UK capabilities in delivering Complex and Innovative Design (CID) studies.
- Watch more related videos our Complex and Innovative Trial Design and Delivery playlist on our YouTube channel: NIHRtv.
- Visit our Delivering Complex and Innovative Research web page to learn more about NIHR support available for complex and innovative trials.

