Published: 30 March 2020
A breathing aid that can help COVID-19 patients with serious lung infections to breathe more easily without the need to use invasive ventilators has been developed by a collaboration of engineers, industry and clinicians.
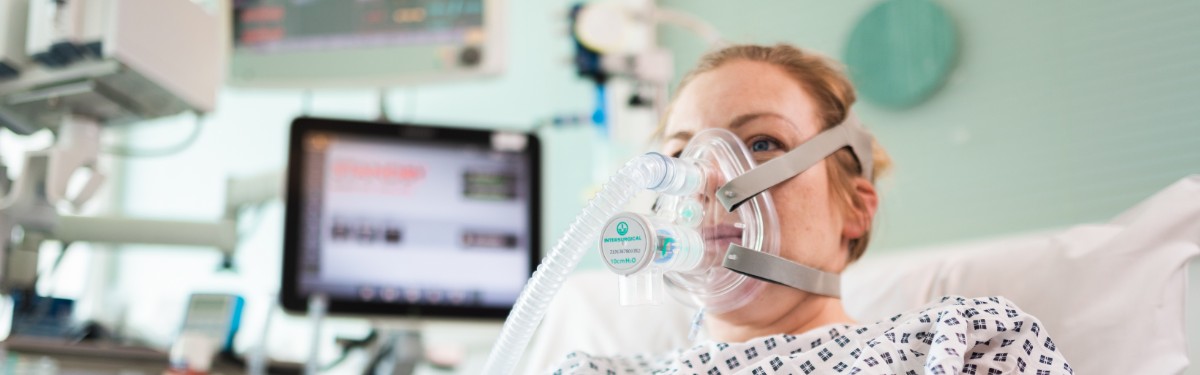
The breathing aid, known as Continuous Positive Airway Pressure (CPAP), has been used extensively in hospitals in Italy and China to help COVID-19 patients with serious lung infections to breathe more easily, when oxygen alone is insufficient.
CPAP machines are used to support patients in NHS hospitals or at home with breathing difficulties. They work by pushing an air-oxygen mix into the mouth and nose at a continuous rate, keeping airways open and increasing the amount of oxygen entering the lungs. Invasive ventilators, on the other hand, deliver breaths directly into the lungs, but require heavy sedation, connection to a tube placed into the patient’s trachea (windpipe) and admission into intensive care.
Reports from Italy indicate that approximately 50% of patients given CPAP have avoided the need for invasive mechanical ventilation, reducing the demand on intensive care staff and beds.
Engineers at UCL, clinicians supported by NIHR UCLH Biomedical Research Centre, and Mercedes AMG High Performance Powertrains (Mercedes AMG HPP) have been working round the clock to reverse engineer a device that can be produced rapidly and manufactured in the thousands. The breathing aid was produced in less than 100 hours from the initial meeting to production of the first device.
The technology has now been approved for clinical and one hundred devices will be delivered to UCLH for clinical trials, with rapid roll-out to hospitals around the country ahead of the predicted surge in COVID-19 hospital admissions.
UCLH critical care consultant Professor Mervyn Singer (UCL Medicine) said: “These devices will help to save lives by ensuring that ventilators, a limited resource, are used only for the most severely ill.
“We hope they will make a real difference to hospitals across the UK by reducing demand on intensive care staff and beds, as well as helping patients recover without the need for more invasive ventilation.”
Professor Bryan Williams, Director of the NIHR UCLH Biomedical Research Centre, said: “This is a fantastic example of collaboration across the UK life sciences and industry sector that could only have happened this quickly because of the partnerships the BRC has cultivated over many years.”
Read more about this story from the NIHR UCLH Biomedical Research Centre.

