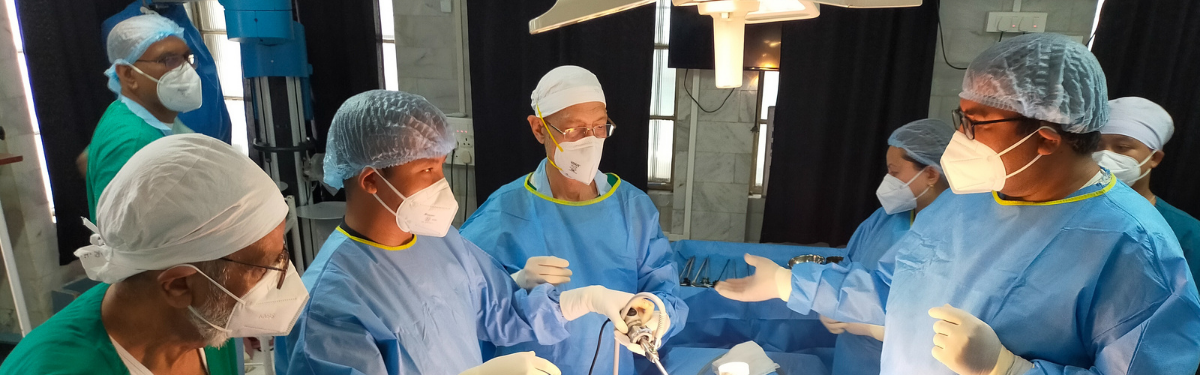
The NIHR Global Health Research Group in Surgical Technologies has developed and trained surgeons to use innovative new devices, enabling routine surgery in remote communities in low-resource settings.
Published: 16 December 2022
Frugal innovations in surgical technology in rural India and Sierra Leone
Only 1 in 10 people in low and middle income countries (LMICs) have any access to basic surgical services. An estimated 11% of the global burden of disease is caused by conditions that are treatable by surgery but those with greatest need often have the least access.
Technology is playing an increasingly important role in delivering surgery globally but surgeons in LMICs are often limited by a lack of high-tech facilities, specialist equipment and general anaesthetics.
In 2017, surgeons and engineers at the NIHR Global Health Research Group in Surgical Technologies at the University of Leeds received £2 million funding to develop innovative technology to improve surgical care in LMICs. Working with partners in northeast India and Sierra Leone, their 3-year research programme identified areas of surgical need and barriers to surgical care.
Led by David Jayne, Professor of Surgery at the University of Leeds, and Professor Julia Brown, Director of Leeds Clinical Trials and Research Unit, the Group focused on two main areas of unmet surgical need: gasless laparoscopy for common abdominal conditions in northeast India and surgery for lower limb fractures and amputation in Sierra Leone.
A revolution in surgical technology in rural India
In rural northeast India, acute abdominal conditions requiring urgent surgery are common. For those patients who can access surgery, laparoscopic (keyhole) methods are preferable to open surgery to reduce the risk of infection and improve recovery times.
The Group’s work, published in BMJ Open, highlighted how rural hospitals were not equipped to undertake laparoscopic surgery and there were too few anaesthetists to supervise general anaesthesia.
A potential solution lay in a modified form of laparoscopic surgery, known as gasless insufflation less laparoscopy. The team developed a gasless laparoscopy training programme at Kolkata Medical Centre for rural surgeons from northeast India (published in the International Journal of Surgery Open). They also established a programme to support new surgeons and a registry to ensure safe adoption of the technique into routine care.
The team also developed an innovative device, the retractor for abdominal insufflation-less surgery (RAIS), to make gasless laparoscopy easier. The RAIS device lifts the abdominal cavity to create an operating space, without using expensive carbon dioxide gas, and can be performed under spinal anaesthesia without an anaesthetist present.
Their results, published in the IEEE Journal of Translational Engineering in Health and Medicine, confirmed that the device made low-cost laparoscopic surgery possible in rural areas. It was also less costly than traditional open surgery (PLOS ONE).
“Providing laparoscopic surgery can help rural patients get back to work as soon as possible. This is vital because the longer they take to recover, the higher the chance of them falling below the poverty line.”
Dr Jesudian Gnanaraj, a urologist at Karunya University, and lead researcher for the project in India
This ‘frugal’, cost-effective innovation has now been rolled out across rural hospitals in northeast India, with the Association of Rural Surgeons of India supporting surgeons’ training in gasless laparoscopy at four key sites in India. It now also monitors the gasless laparoscopy registry as the technology is adopted in other areas.
The Group’s results have been widely shared with national policy makers and global health organisations, influencing decisions around surgical care provision. They later secured separate funding from the UK Research and Innovation Global Challenges Research Fund to progress the RAIS device towards commercialisation and take the gasless laparoscopy training programme into Kenya’s network of rural training hospitals.
The team went on to secure an industry partner for the RAIS device in India (XLO Ortho Life Systems), enabling the device to be manufactured in-country. Their low-cost laparoscopic simulator (LapPack), specifically designed to be viewed via mobile devices to assist with surgeons’ training, will support training in other LMICs and make surgery more accessible.
Improving lower limb surgery outcomes in Sierra Leone
In Sierra Leone, the Group’s research focused on the increasing problem of lower leg fractures. Working with the College of Medicine and Health Sciences at the University of Sierra Leone and Connaught Hospital in Freetown, they undertook a clinical trial (FIXT) to assess a new method for treating lower leg fractures.
The trial compared the outcomes of 20 patients treated using the low-cost Ilizarov frame fixation method (using metal pins and an external frame) with 20 others who received usual care (bed rest and skin traction). The results will show whether Ilizarov frame fixation improves healing and recovery rates, providing evidence for an improved and cost-effective technique for other low-resource settings.
The method is already used by some hospitals in Sierra Leone and the team secured additional funding from the British Medical Association Foundation to improve the existing technology.
A second project (the VITAL trial) in Freetown, Sierra Leone, showed how surgeons demonstrated better amputation skills following virtual reality training than those using the standard learning materials. If used in practice, this method has far-reaching implications for many other clinical training settings.
With the assistance of Dr Ibrahim Bundu at the University of Sierra Leone and lead researcher for the project in Sierra Leone, the team worked closely with the West African College of Surgeons and the Medical and Dental Association of Sierra Leone to raise awareness of their research and new techniques nationally.
“It has been exciting to be a part of this NIHR Global Health Research initiative. This is a great example of team science, where difference skill sets are brought together to solve some of the most pressing needs in the most challenging environments.”
Professor David Jayne
The research was funded by the NIHR Global Health Research Programme through Official Development Assistance (ODA) from the UK aid budget.

