NIHR Programme Grants for Applied Research (PGfAR) is seeking to increase the diversity of study type and design submitted for funding. This case study proposes a innovative research design to improve the use of data from stroke patients to drive improvements in stroke care.
Programme details
Programme name: Improving the lives of stroke survivors with data
Researcher name: Professor Charles Wolfe
Institution: Guy’s and St Thomas’ NHS Foundation Trust
Funding: £2,195,908
Benefits to patients and the NHS
This research will address key gaps identified by the Long Term Plan (LTP) for improving stroke care. The need for better information about the long-term consequences of stroke was highlighted by the James Lind Alliance as a priority.
The following benefits are anticipated for stroke survivors and the NHS, within the programme’s five-year timeframe:
- Health care improvements driven by stroke survivors, their families and stakeholders ensuring that stroke care is fit for purpose
- Changes to local and national health policy, to better meet the needs of stroke survivors in the 2020s
- Ability of policy makers, commissioners, and clinicians to base decisions on up to the minute and accurate data on stroke risk and outcomes
- Improved access for patients to their own health data, aiming to ensure that they are involved in their decision making
Aims of the programme
- To maximise the potential for stroke data to improve patient care through stakeholder engagement
- To estimate the risk and longer term impact (including economic) of stroke on survivors and society
- To produce clinical, epidemiological and economic models which will provide the information needed for all stakeholders to make informed decisions
- To investigate how patient portals can improve stroke survivors’ decision making and outcomes
Programme design
The programme is structured around three work packages, which include work with stroke survivors and their families, health professionals, policy makers and commissioners of health services, and technologists. These work packages will be interlinked (see Figure), in order to ensure that the outputs are relevant to all stakeholders. By doing this, we will make sure that we are analysing data in the most useful way; ensure that patient portals are usable by stroke survivors who may have complex disabilities; and have the greatest chance of translating into improved health care and policy.
Figure 1 - Programme work packages
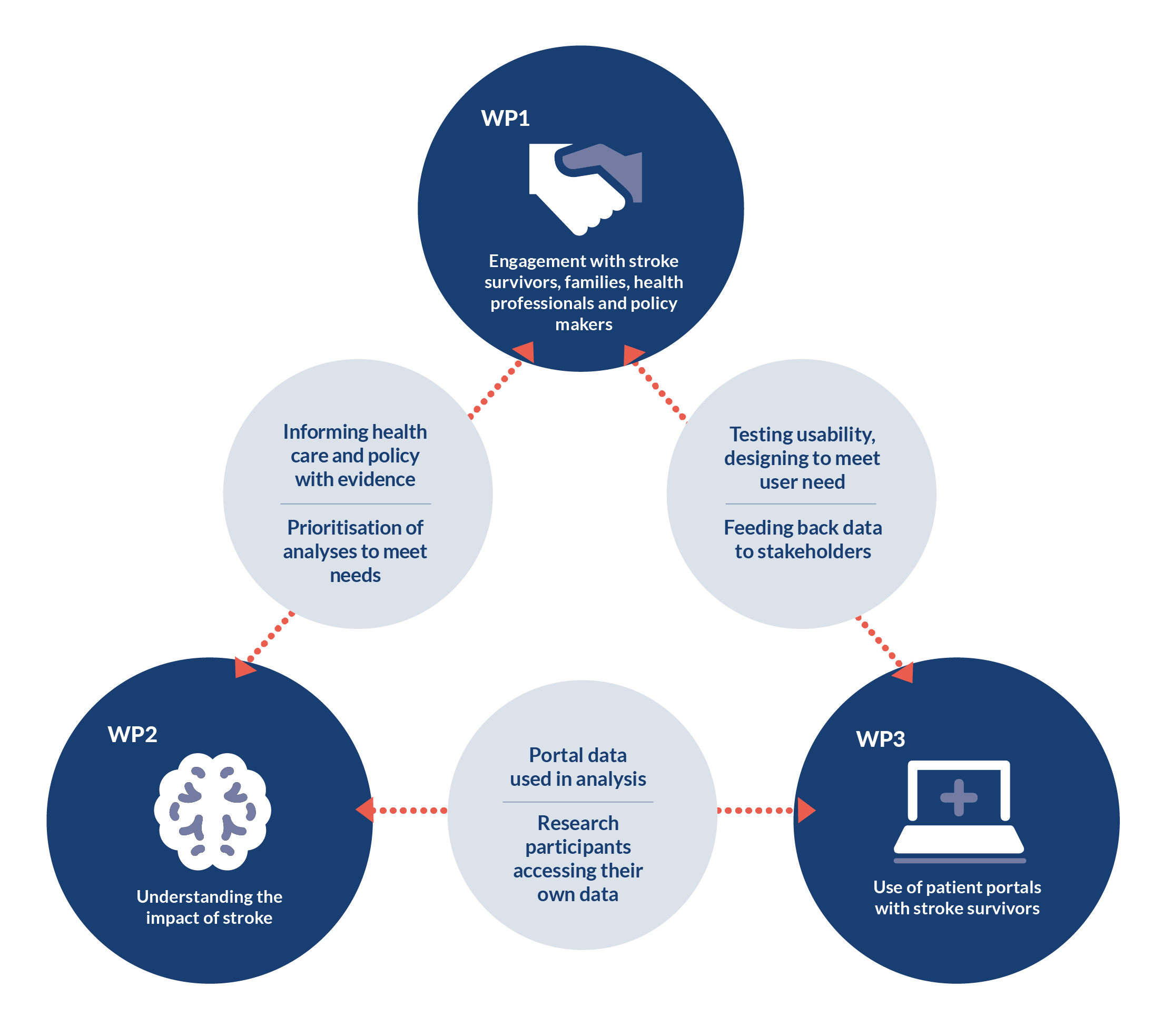
Work package 1: Maximise the potential for stroke data to improve care
This work package will utilise social science and policy methods to ensure that the expertise, lived experiences, attitudes and needs of the full range of stroke survivors in society, carers, healthcare professionals and policy makers are embedded across the programme and its decisions, outputs and impact activities.
Methods: Collect and analyse qualitative data on the planned data collection, analyses and methods of dissemination of findings from patient and stakeholder groups.
Work package 2: Investigate the impact of stroke on survivors in the 2020s
This work package will expand the South London Stroke Register (SLSR) data collection to address and conduct analyses to answer key questions, informing health care and policy to meet patient needs.
Methods: Collection and analysis of prospective and historical data from the SLSR and comparison with Oxford Vascular Study (OXVASC) data.
Work package 3: Investigate how patient portals can improve the care of stroke survivors
This work package will build on the achievements of the King’s CONSULT (Collaborative mObile decisioN Support for managing mULTiple morbidities) stroke patient portal. The patient portal functionality will be evaluated in feasibility trials and its cost-effectiveness modelled.
Methods: Building on the CONSULT software architecture, a visualisation methodology will be adapted using established models and theories of visual communication to ensure the portal’s efficacy, usability and accessibility. Components of the patient portal will be evaluated via four embedded feasibility randomised trials, which will explore the effect of portal usage on different subgroups of SLSR patients who will be able to access their own data. An online dashboard will be developed to complement the patient portal and facilitate uptake of the project’s findings and serve as an information centre for policy makers, the research community and wider public. Data will be collected on the costs of the portal development, use and maintenance to inform the economic model.

