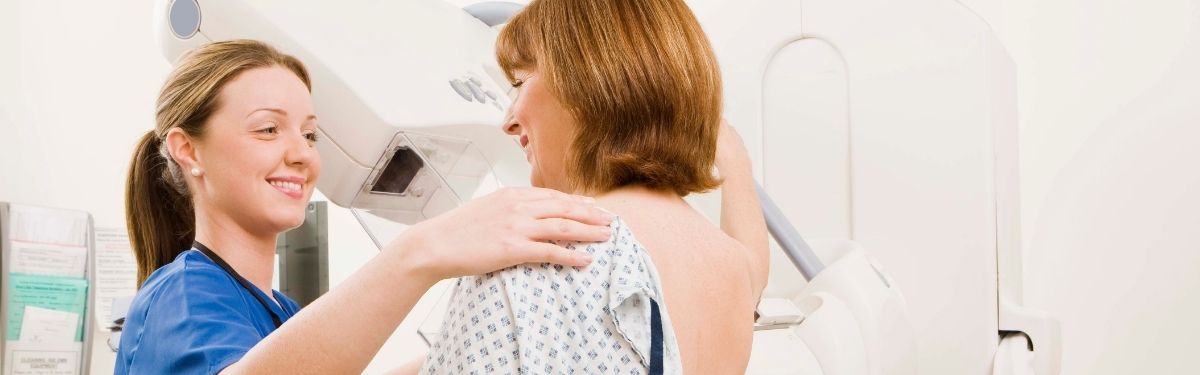
Screening women for breast cancer in their forties reduces their chance of dying from breast cancer by 25% in the first 10 years of screening.
Published: 01 December 2020
Only women over 50 are currently offered routine breast screening
The UK’s current breast cancer screening programme offers mammograms to women aged between 50 and 70 years every three years. However, it is still unclear whether screening women from 40 years old is beneficial. Women in their forties are not routinely invited for screening because their risk of developing breast cancers is lower. However, the types of cancers that do develop in younger women are often more aggressive and progress more quickly. In these cases, earlier diagnosis and treatment would greatly benefit those patients.
Recently published research from the long-term NIHR-funded UK Breast Screening Age Trial (UK Age Trial) provides further evidence of the benefits and risks of earlier screening for women. Led by Professor Stephen Duffy, the trial began in 1990 and randomly assigned 160,000 women aged 39–42 to receive annual mammography or the usual NHS Breast Screening Programme. These women have now been followed up for around 23 years and the latest results have been published in The Lancet Oncology.
Evidence of benefit for women in their forties
After 23 years of follow up, the trial has shown that regular screening of women aged 40–49 reduced their chances of dying from breast cancer during the first 10 years by 25%. This equated to around one breast cancer death being prevented for every 1000 women screened. Although deaths from breast cancer were not reduced further once women began regular mammography screening at the age of 50, 11.5 years of life were saved per 1000 women who were screened in their forties.
While screening gives doctors the opportunity to diagnose and treat breast cancer earlier, when it is easier to treat and with fewer side effects, there is also a concern that some breast cancers may be over-diagnosed. This occurs when early cell changes that may not go on to cause life-threatening disease are diagnosed as a cancer and are unnecessarily treated. Reassuringly, the study found that there was little overdiagnosis additional to that which would occur from screening women in their fifties in the national programme. Stephen Duffy, Professor of Cancer Screening at Queen Mary University of London, commented:
"Breast cancer does not respect one’s 50th birthday. In the past, there has been a tendency to think of the issue in binary terms: that the screening does not work before age 50 and does after. We can now see that it works from age 40 upwards, but does not work as well in terms of absolute numbers of breast cancer deaths prevented in women under age 50."
Dr Imogen Locke, Consultant Clinical Oncologist at The Royal Marsden NHS Foundation Trust, said: “This important study suggests that offering mammographic screening to women from a younger age results in breast cancers being detected at an earlier and more curable stage. Diagnosing breast cancers before they cause symptoms results in fewer women dying from breast cancer and may also mean that women require less aggressive cancer treatment. We are continuing to see the importance of early diagnosis and screening across breast and other types of cancer too.”
Helping to guide national and international public health and research
The UK Age Trial team have contributed their data and expertise to a number of breast cancer screening groups to support improvements in healthcare through screening. Professor Duffy was invited to join the Clinical Advisory Group for the 2018 breast screening incident, in which a number of women eligible for screening through the NHS Breast Screening Programme didn’t receive invitations. By providing details of the likely effects of the incident and of the actions planned to help rectify the situation to, the advisory group has made decisions that will inform future practice within the NHS Breast Screening Programme. This includes systems to ensure that all eligible women receive their screening invitations.
The UK Age Trial has also had international impact, with its results contributing to recommendations in the 2019 European Breast Cancer guidelines stating that mammography screening should be offered to detect early breast cancer in women aged 45–49 years. Professor Duffy was a member of the guidelines development working group.
The research team has an ongoing collaboration with Radboud University in The Netherlands, in which they have assessed how well different study design methods (such as case-control and randomised controlled trials) measure the effectiveness of new breast cancer screening techniques. The understanding gained from the research will help inform improvements to breast cancer screening programmes in the UK and other countries in the future.
Members of the Rotterdam-based Cancer Intervention and Surveillance Modelling Network are using data from the UK Age Trial and several other screening trials to help predict how effective a range of mammography screening policies may be. The models they produce will be used to guide public health research and to develop the most effective approaches to screening for cancers.
Identifying further research for future screening
As the UK Age Trial began 23 years ago, several advances have been made in the technology used to detect early cancer since the trial’s screening phase took place in the 1990s and early 2000s. During this time, screen-film mammography has been replaced by digital mammography and screening protocols have been standardised. Professor Shirley Hodgson, Professor of Cancer Genetics, St George’s, University of London, said: “There is clear evidence from this study that mammography screening from 40 years of age has the potential to save lives from breast cancer. The fact that early screening involves annual screens, which at the time of the study were less sensitive than those done nowadays, indicates that the sensitivity of screening may be greater now, but possibly this could result in more false positive diagnoses.”
The UK Age Trial team acknowledges that further research focusing on the effect of screening with modern imaging techniques is needed in this age group to clarify this, alongside the possibility that improvements in breast cancer treatment during this period could further reduce the number of deaths. Professor Duffy said: “In the future, further evaluation of the economics, affordability and acceptability of screening by age will be needed. However, now is not the time to be expanding the target population, as the programme’s first priority must be to meet the capacity challenges arising partly as a result of the COVID-19 pandemic.”
The study was funded by NIHR’s Health Technology Assessment (HTA) Programme.
More information about the study is available on the NIHR’s Funding & Awards website.

